New Life & Health Narrative: Meeting Underwriters At Every Step
.png)
Life & Health underwriting is a constant balance between speed and quality: getting the right coverage to customers before they go somewhere else. One missed detail can change the whole quote. But the longer pricing takes, the greater the risk of applicant drop-off.
Accelerated underwriting helps with simpler cases that don't require additional evidence, but as recently reported by Gen Re, up to 88% of cases still need some type of human review.
Those cases still go through the same workflow: sorting through documents at initial review, going back to the advisor or broker when something's missing, and when the case is finally ready, reading through hundreds of pages of medical records like EHRs, APS, and lab results to piece together the full health picture before making a decision.
It's a lot of steps and a big manual workload that keeps underwriters from bringing in more premiums and getting back to customers faster with better coverage. That’s where Sixfold comes in; underwriting AI built to help at every step of the process, bringing together the details that matter to your team, and now with our new Narrative, a tailored initial analysis that simplifies triage and reduces the unnecessary back and forth, before the deeper analysis.
The First Look At a Case
At the initial review, underwriters are trying to answer one question: Do I have what I need to move this case forward? Most of the time, that means going through multiple documents just to find out, and when something's missing, at least 30 minutes are spent on a case they'll have to come back to later.
Our new Narrative capability for Life & Health is a focused, structured case summary tailored to what matters to your underwriting team, surfacing the information you want to see upfront to help underwriters with triage and to figure out next steps. Sixfold’s AI agents read through all the case documents, application, APS, MIB, and labs, and pull together the relevant details into one structured view, so underwriters don't have to. Each narrative is configurable to your team's specific workflow, so what gets surfaced reflects what actually matters for your decisions.
Imagine a case where an applicant has hypertension or a history of elevated cholesterol. The underwriter immediately needs to know if they have all the information about blood pressure and what meds they're on. Does this applicant smoke? What is their family history? This is information they need before they even begin to assess the case.
The Narrative gives you exactly the information you need to know before you move on.
"We want to support underwriters at every point in their workflow. Sometimes that means a focused Narrative to help with triage and next steps. Sometimes that means a deep condition analysis across hundreds of pages. The point is, wherever an underwriter is in the process, Sixfold is there to help."
— Noah Grosshandler, Product Manager at Sixfold
On the reinsurer side, it's a similar story. Underwriters are spending precious time just organizing loosely assembled submissions from cedents because most times the cases come in an inconsistent format, requiring additional questions before quoting, many of which wouldn't even be necessary if the information were clearly structured upfront.
With Narrative, these questions are answered upfront. Fewer emails back and forth with brokers and faster responses.
The Full Clinical Story: Conditions Analysis
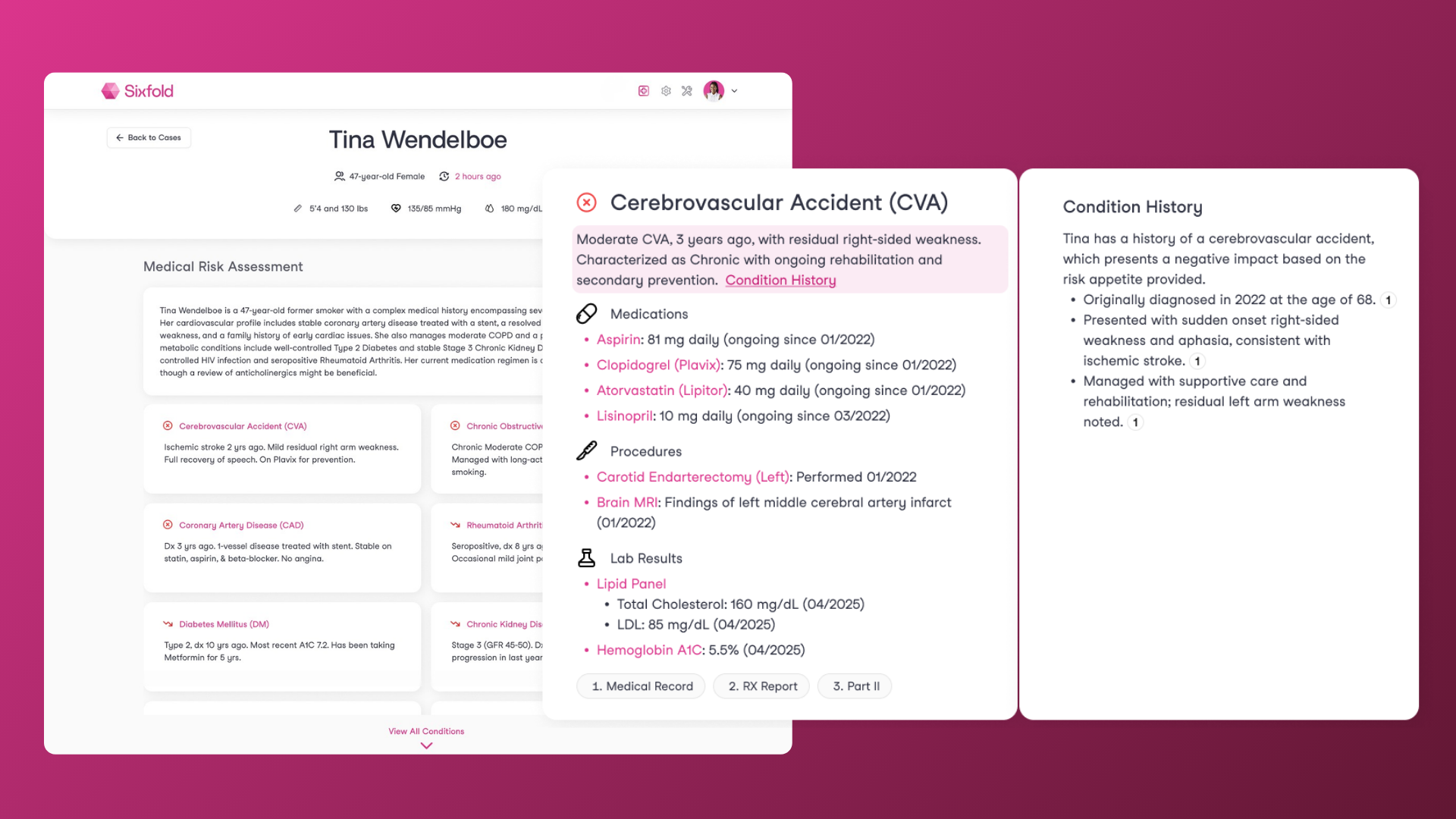
After triaging and making sure a case is ready to quote, underwriters go back to the manual review of hundreds of pages of medical records, trying to spot that one detail that will change the whole quote. It's pretty much like detective work, finding how a medicine connects to a diagnosis and what the impact is on that patient, trying to piece together the full medical story. Assessing history, severity, and how well a diagnosis is managed. Meanwhile, customers are waiting for a response.
That's where Sixfold's in-depth Conditions Analysis comes in. When the case is ready for a full review, our Conditions Analysis connects all the medical pieces, bringing together medications, labs, procedures, and diagnoses under each condition so underwriters can see the full clinical picture without jumping between documents. It highlights what's relevant to your underwriting guidelines, shows how conditions have progressed over time, and surfaces the clinical data that matters most for your decisions.
One example is a case where an applicant is taking Spironolactone, a common medication used to control high blood pressure, but also prescribed for hormonal acne. An underwriter would have to go through lengthy pages of documentation to find what dosage they're on, how long they've been taking it, and what it's actually being prescribed for. And that's just one medication. For complex cases, underwriters are doing this across multiple conditions with years of medical history.
With our Conditions Analysis, underwriters can spend their time on decision-making rather than document review and data gathering. Customers get faster and better quotes. Guardian, for example, saw a 50% reduction in review time using Sixfold.
When Speed is What Matters
Some of our customers work with higher-volume lines like structured settlements and annuities and often process over 10,000 cases per year; they don’t always need an in-depth Condition Analysis to move a case to the next step.
There are fewer key risk details that influence the analysis, so they have been able to use Narrative to move forward on up to 70% of their cases, consulting our full Conditions Analysis only for the most complex ones. For some teams, Narrative handles most of the heavy lifting of manual review.
"One of our customers built Narrative into their workflow for initial case review. It helps their underwriters get up to speed quickly and know exactly what needs attention. When a case requires deeper analysis, they move to our full Conditions Analysis, but Narrative gives them that strong starting point." — Justin Sorce, Customer Success Manager at Sixfold
Confident Underwriting Decisions
Whether it's a quick initial review or a deep dive into a complex case, Sixfold is there to help your team get to a confident underwriting decision faster.
And it works where your team already works, whether that's in our UI, a workbench, or a policy admin system. Every insight ties back to the source documents, so underwriters can verify what they're seeing. Built for underwriting since day one. HIPAA and SOC 2 certified, with single-tenant environments to keep your data secure. Rigorous AI fairness testing to meet evolving regulatory standards and grounded in our Responsible AI principles.

